|
The measurement of respiratory function is important in the hospital setting as it relates to numerous disease states and may be indicative of ensuing issues. Future work should aim to further test these parameters in the clinical setting. In addition, a high degree of correlation between depth-based tidal volume and its ventilator reference was found, indicating that TV depth may provide a useful monitor of tidal volume trending in practice. 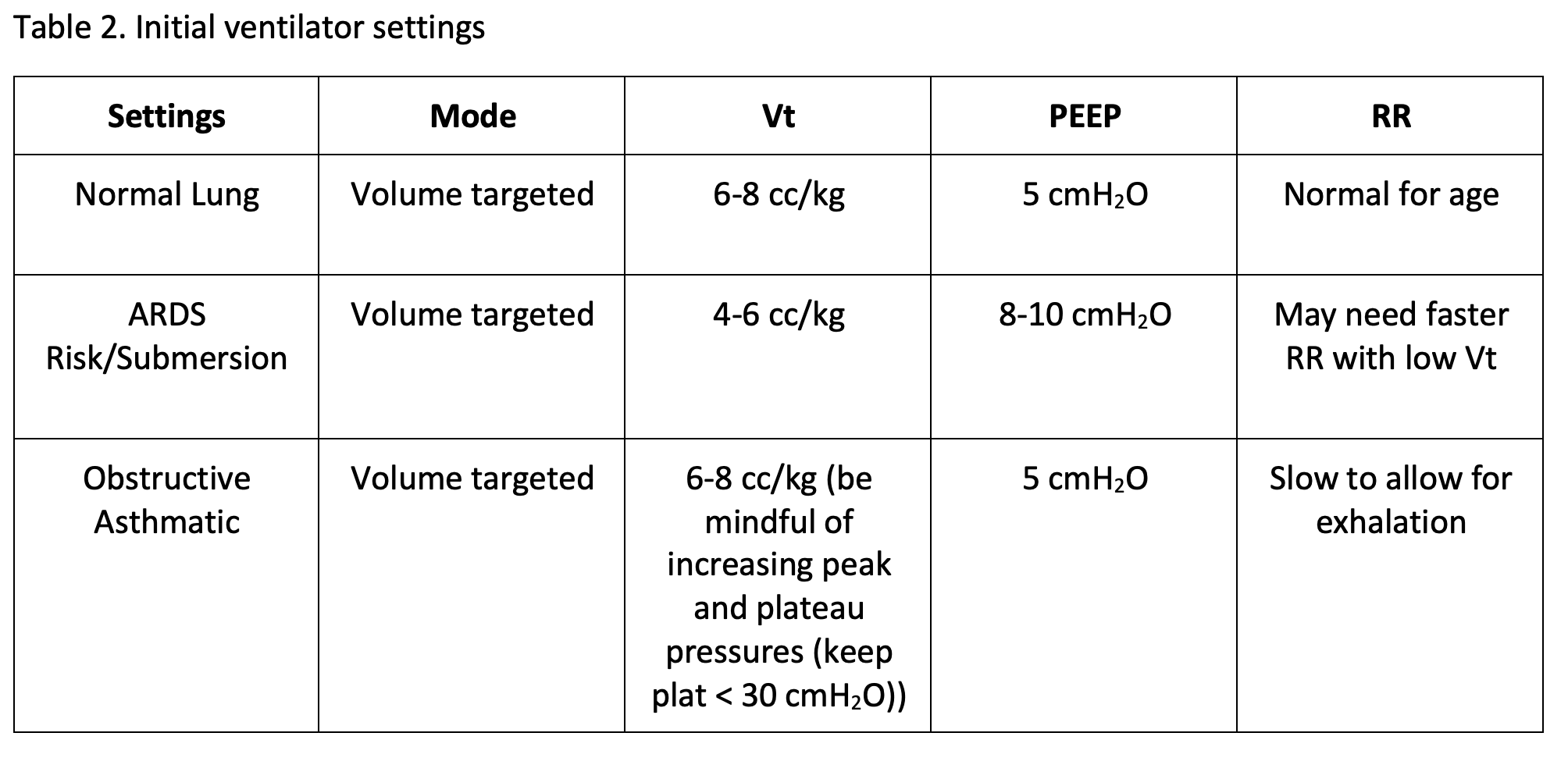
In conclusion, a high degree of agreement was found between the depth-based respiration rate and its ventilator reference, indicating that RR depth is a promising modality for the accurate non-contact respiratory rate monitoring in the clinical setting. The least squares fit regression equation was determined to be: TV depth = 0.79 × TV vent-0.01 L and the resulting Pearson correlation coefficient, R, was 0.92 (p < 0.001). Correspondingly, the bias and root mean squared difference (RMSD) accuracy between TV depth and the reference TV vent across the whole data set was found to be − 0.21 L and 0.23 L respectively. The least squares fit regression equation was determined to be: RR depth = 0.96 × RR vent + 0.57 breaths/min and the resulting Pearson correlation coefficient, R, was 0.98 (p < 0.001). The bias and root mean squared difference (RMSD) accuracy between RR depth and the ventilator reference, RR vent, across the whole data set was found to be -0.02 breaths/min and 0.51 breaths/min respectively. Depth sensing data streams were acquired and processed over a series of runs on a single volunteer comprising a range of respiratory rates and tidal volumes to generate depth-based respiratory rate (RR depth) and tidal volume (TV depth) estimates. Here we report on the performance of a depth-sensing camera system for the continuous non-contact monitoring of Respiratory Rate (RR) and Tidal Volume (TV), where these parameters were compared to a ventilator reference. 1–24.The monitoring of respiratory parameters is important across many areas of care within the hospital. 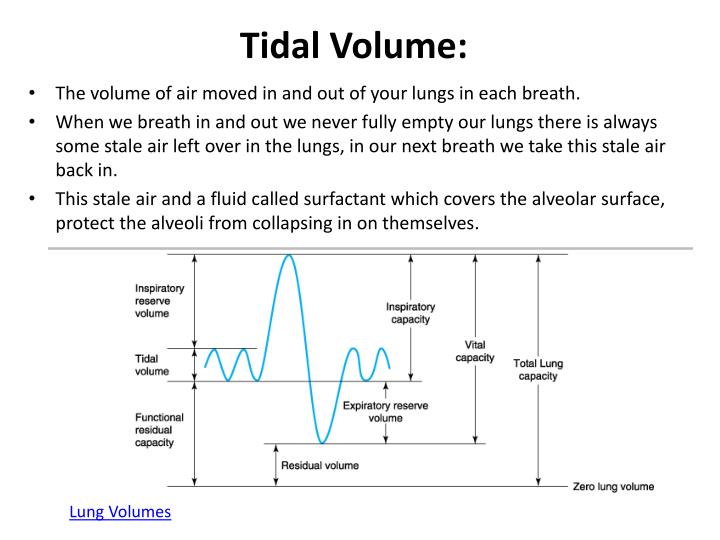
Patterns of unexpected in-hospital deaths: a root cause analysis. Early warning system scores for clinical deterioration in hospitalized patients: a systematic review. Smith MEB, Chiovaro JC, O’Neil M, Kansagara D, Quiñones AR, Freeman M, et al. Protecting ward patients: the case for continuous monitoring. Multicenter study validating accuracy of a continuous respiratory rate measurement derived from pulse oximetry: a comparison with capnography. doi: 10.1097/ALN.0b013e3181c38c25.īergese SD, Mestek ML, Kelley SD, McIntyre R, Uribe AA, Sethi R, et al. Incidence, reversal, and prevention of opioid-induced respiratory depression. Future work should aim to further test these parameters in the clinical setting.ĬOVID-19 Depth sensing camera Respiratory function Respiratory rate Tidal volume.ĭahan A, Aarts L, Smith T. 
The least squares fit regression equation was determined to be: TV depth = 0.79 × TV vent-0.01 L and the resulting Pearson correlation coefficient, R, was 0.92 (p < 0.001). Correspondingly, the bias and root mean squared difference (RMSD) accuracy between TV depth and the reference TV vent across the whole data set was found to be - 0.21 L and 0.23 L respectively. The least squares fit regression equation was determined to be: RR depth = 0.96 × RR vent + 0.57 breaths/min and the resulting Pearson correlation coefficient, R, was 0.98 (p < 0.001). 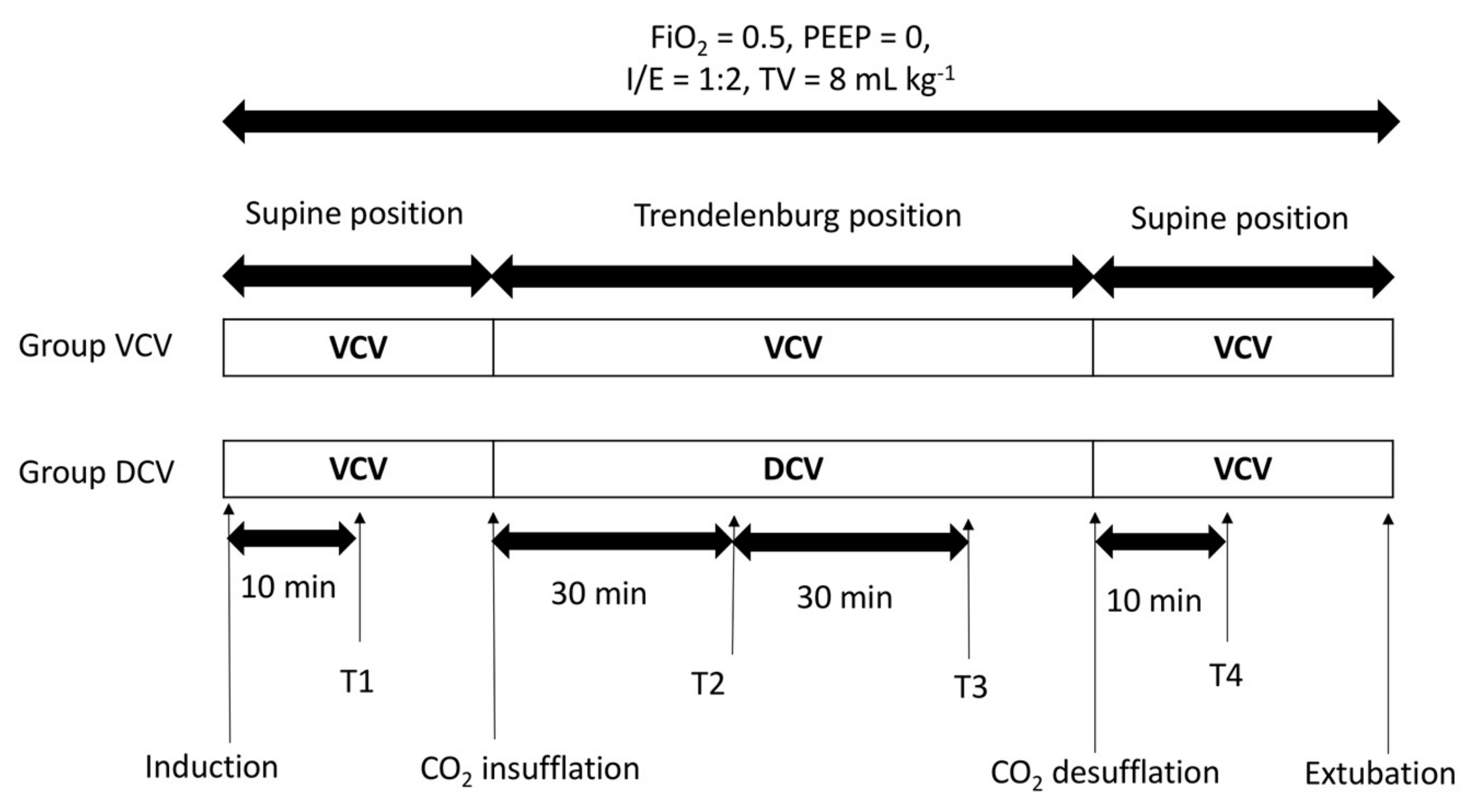
The monitoring of respiratory parameters is important across many areas of care within the hospital.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
